There are 2 main types of skin cancer - non-melanoma skin cancer and melanoma skin cancer.
Non-melanoma skin cancer is also known as keratinocyte cancer. It is one of the most common cancers in the world. More than 13,000 people are diagnosed with it each year in Ireland.
Non-melanoma skin cancer affects more men than women. It is more common among people age 65 and older.
Non-melanoma skin cancer is much more common than melanoma skin cancer.
Symptoms of non-melanoma skin cancer
The first sign of non-melanoma skin cancer is usually a lump or crusted area of skin that has not healed.
It does not go away and slowly progresses over months or sometimes years.
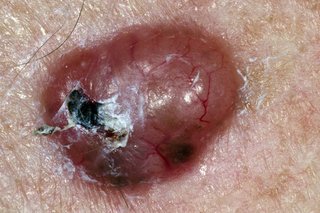
Non-melanoma skin cancer often develops on areas of skin that are in the sun a lot.
These include your:
- face
- ears
- hands
- upper chest
- neck
When to get medical advice
Non-urgent advice: Go to your GP if:
you have noticed any skin change
This could be a:
- lump that is tender and grows quickly
- a cut or break in the skin that does not heal after a few months
While it's not likely to be skin cancer, it's best to check it out.
Types of non-melanoma skin cancer
Non-melanoma skin cancers usually develop in the outer layer of skin (epidermis). There are different types of cells in the epidermis. These include basal cells and squamous cells.
The 2 most common types of non-melanoma skin cancer are:
- basal cell carcinoma (BCC)
- squamous cell carcinoma (SCC)
Basal cell carcinoma
Almost 2 in 3 skin cancers are BCC.
BCC starts in the cells lining the bottom of the epidermis. It usually appears as a small, shiny pink or pearly-white lump - sometimes with bits of brown or black in it. The lump grows slowly. It may become crusty or bleed and does not heal. Or it may develop into a painless ulcer (broken area of skin).
BCC can also look like a red, scaly patch.
Squamous cell carcinoma
About 1 in 4 skin cancers is SCC.
SCC starts in the cells lining the top of the epidermis. It appears as a firm pink or skin-coloured lump with a rough or crusted surface. Sometimes there is a spiky horn sticking up from the surface.
The lump is often tender to touch and may bleed. It may develop into an ulcer.
Pre-cancerous growths
There are pre-cancerous growths that may develop into non-melanoma skin cancer if they are not treated.
These include:
- Bowen's disease
- Actinic keratoses
Bowen's disease
Bowen's disease is also called squamous cell carcinoma in situ. It develops slowly and is easy to treat.
The main sign is a red, scaly patch on the skin. It may be itchy. It can appear on any area of the skin. In women, it is often found on the lower legs.
It can develop into SCC.
Actinic keratoses
Actinic keratoses are dry, scaly patches of skin. They are also known as solar keratoses. They are caused by the skin being exposed to the sun for a long time.
You may have a lot of these patches. They can be pink, red or brown. They can vary in size from a few millimetres across to a few centimetres.
They often appear on parts of your body that have been in the sun a lot. For example, the back of your hands or your scalp.
The affected skin can sometimes become very thick. The patches can look like small horns or spikes.
There is a small risk of them developing into SCC.
Diagnosing non-melanoma skin cancer
Your GP can examine your skin for signs of skin cancer.
They may refer you to a specialist if they're unsure or suspect skin cancer. This could be a dermatologist (also called a skin specialist) or a plastic surgeon.
SCC needs more urgent attention than BCC or pre-cancerous skin changes.
Skin examination
The dermatologist or plastic surgeon will examine your skin. They may carry out a biopsy (take a small sample of the skin) to help them make a diagnosis. Or they may remove the affected area - this is called an excision.
These procedures are carried out under local anaesthetic. This means the area will be numbed, so you will not feel any pain.
After the biopsy or excision, the sample is sent to the laboratory to be examined under a microscope.
The test will tell if you have skin cancer and the type of skin cancer it is.
If your specialist removes the affected area, you may not need more treatment.
Other tests you might need
If you have BCC, it is very unlikely that the cancer will spread. You will not usually need more tests.
But if you have SCC, it can spread. This is rare. If the cancer spreads, it may cause your lymph nodes to swell. Your specialist will examine your lymph nodes.
Sometimes they will take a sample from a lymph node. This is called a fine needle aspiration (FNA) or a core biopsy. Cells are removed from the lymph node using a needle and syringe. They are examined under a microscope.
In rare high-risk cases of SCC, you may need an ultrasound or CT scan - this is called a staging test. It will check if the cancer has spread to the lymph nodes or to another part of your body.
Content supplied by the NHS and adapted for Ireland by the HSE
