Hidradenitis suppurativa (HS) is a painful skin condition that causes abscesses and scarring on the skin.
The exact cause of hidradenitis suppurativa is unknown, but it happens near hair follicles where there are sweat glands. This is usually around the groin, bottom, breasts and armpits.
Hidradenitis suppurativa affects about 1 in 100 people. It is more common in women than men.
Symptoms
The symptoms of hidradenitis suppurativa range from mild to severe.
It causes a mixture of:
- boils
- blackheads
- cysts
- scarring
- channels in the skin that leak pus (called sinuses)
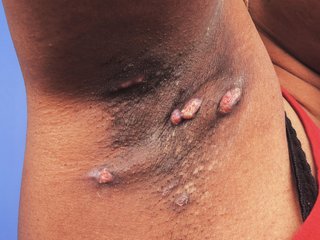
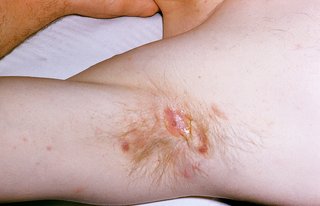
Hidradenitis suppurativa starts with a boil that develops in one place. This will either disappear or rupture and leak pus after a few hours or days.
New boils will then often develop in an area nearby. If these are not treated with medicine, larger lumps may develop and spread. Narrow channels also form under the skin that break out on the surface and leak pus.
The boils develop on the skin:
- in the armpits
- below the breasts
- around the groin and genitals
- on the bottom and around the anus
The condition may also spread to your:
- neck
- face
- back area
- waistband
- inner thighs
- front or back of the legs
Some of the lumps may become infected with bacteria. This can cause a secondary infection that will need to be treated with antibiotics.
What causes hidradenitis suppurativa
The exact cause of hidradenitis suppurativa is unknown. But the lumps develop as a result of blocked hair follicles.
Hidradenitis suppurativa runs in families in about 1 in 3 cases. It's not infectious and is not linked to poor hygiene.
Smoking and obesity are both strongly associated with hidradenitis suppurativa. If you have obesity or smoke it will make your symptoms worse.
Hidradenitis suppurativa usually starts around puberty, but it can happen at any age. It's less common before puberty and after the menopause. This may suggest that sex hormones play a part. Many people with the condition also have acne and excessive hair growth (hirsutism).
In rare cases, hidradenitis suppurativa may be linked to Crohn's disease, particularly if you get it around the groin area and the skin near your bottom.
Diagnosing hidradenitis suppurativa
There's no one test diagnose hidradenitis suppurativa.
Your GP will examine the affected areas of skin. They may take a swab of an infected area. This can be helpful in making a diagnosis.
Hidradenitis suppurativa can be mistaken for acne or ingrown hairs.
Treating hidradenitis suppurativa
Hidradenitis suppurativa can be a lifelong, recurring condition that is difficult to manage.
It's important to recognise and diagnose the condition in its early stages. This can help prevent it getting worse.
In the early stages, it may be controlled with medicine. You may need surgery if your case is severe or keeps returning.
Antibiotics
If you have lumps that are particularly painful, inflamed and oozing pus, you may be prescribed a 1 or 2 week course of antibiotics, as you may have an infection. But in hidradenitis suppurativa, a secondary bacterial infection is not that common. Your GP should do a swab of the affected area.
If you do not have a bacterial infection, your GP may suggest low doses of antibiotics to prevent inflammation. This longer course of antibiotics will last at least 3 months, to reduce the number of lumps that develop.
You may be given antibiotics as a cream (topical) or as a tablet, capsule or liquid.
In severe cases of hidradenitis suppurativa, a combination of clindamycin and rifampicin can be effective. But these antibiotics are usually prescribed by dermatologists rather than your GP.
Antiseptics
Antiseptic washes such as 4% chlorhexidine are often prescribed alongside other treatments. These can be used to clean the affected areas on a daily basis.
Retinoids
Retinoids, such as isotretinoin and acitretin, are vitamin-A based medicines. They are usually prescribed for acne. They are not as effective for treating hidradenitis suppurativa. But they may help you.
Retinoids are always prescribed by dermatologists. They must be used with caution.
Do not take retinoids if you are pregnant or think you may be pregnant.
Contraceptives
If hidradenitis suppurativa flares up before your period you may benefit from taking the combined contraceptive pill.
Immunosuppressive treatments
In severe cases of hidradenitis suppurativa, treatments that suppress the immune system can be useful. These include adalimumab and infliximab.
But there are risks associated with suppressing the immune system. These treatments are usually only prescribed by a dermatologist if other treatments do not work.
Infliximab and adalimumab are immunosuppressive treatments that are given by injection at regular intervals either at home or in hospital.
Steroids
Rarely, you may be prescribed steroids such as prednisolone to treat severely inflamed skin. Steroids can be taken as tablets, or you may have an injection directly into affected skin.
Possible side effects of steroids include:
- weight gain
- poor sleep
- mood swings
Surgery
You may be advised to have surgery if your condition cannot be controlled with medicine.
Lifestyle advice
If you have hidradenitis suppurativa you should:
- wear loose-fitting clothes
- hold a warm flannel on the lumps to encourage the pus to drain
- avoid shaving affected skin and avoid wearing perfume or perfumed deodorants in the affected areas
- stop smoking (if you already smoke)
Living with hidradenitis suppurativa
Hidradenitis suppurativa can continue for many years. But if it's diagnosed early your symptoms can be improved with treatment.
The condition can have a significant impact on your everyday life. Having to regularly change dressings and live with the pain and discomfort can affect your quality of life.
Speak to your GP if you're finding it difficult to cope.
Content supplied by the NHS and adapted for Ireland by the HSE