Cellulitis is a common bacterial skin infection that's treated with antibiotics. It can be serious if it's not treated.
Symptoms of cellulitis
The affected skin appears swollen and red and is painful and warm to touch. If it is not treated, the infection can spread to the lymph nodes and can quickly become life threatening.
You can get cellulitis on any part of your body, but it usually affects:
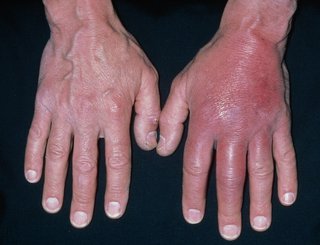
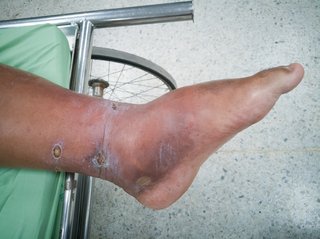
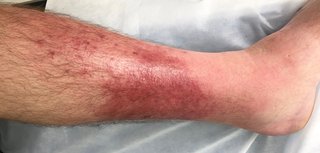
Urgent advice: Ask for an urgent GP appointment if:
- your face or the area around your eye is affected
- your symptoms are rapidly getting worse
- you have a weakened immune system – for example, because of chemotherapy or diabetes
- a young child or elderly person has possible cellulitis
Early treatment with antibiotics can stop the infection from becoming more serious.
Causes of cellulitis
Cellulitis is usually caused by a bacterial infection. The bacteria can infect the deeper layers of your skin if it's broken. For example, because of an insect bite or cut, or if it's cracked and dry.
Sometimes the break in the skin is too small to notice.
You cannot catch cellulitis from another person as it affects the deeper layers of the skin.
You're more at risk of cellulitis if you:
- have poor circulation in your arms, legs, hands or feet
- find it difficult to move around
- have a weakened immune system because of chemotherapy treatment or diabetes
- have bedsores or pressure ulcers
- have lymphoedema, which causes fluid build-up under the skin
- inject drugs
- have a wound from surgery
- have had cellulitis before
People who are more at risk of cellulitis should treat athlete's foot promptly.
Treatment for cellulitis
For mild cellulitis affecting a small area of skin, your GP will prescribe antibiotics – usually for a week.
Your symptoms might get worse in the first 48 hours of treatment but should then start to improve.
It's important to keep taking antibiotics until they're finished, even when you feel better.
Most people make a full recovery after 7 to 10 days.
If your cellulitis is severe, your GP might refer you to hospital for treatment. You will be given fluids and antibiotics intravenously (directly into a vein by injection).
Some people with recurring cellulitis might be prescribed low-dose, long-term antibiotics. This is to stop infections coming back.
Self-management of cellulitis
As well as taking antibiotics, you can help speed up your recovery by:
- taking paracetamol or ibuprofen for the pain
- raising the affected body part on a pillow or chair when you're sitting or lying down to reduce swelling
- regularly moving the joint near the affected body part, such as your wrist or ankle, to stop it getting stiff
- drinking plenty of fluids to avoid dehydration
- not wearing compression stockings until you're better
You can reduce the chances of getting cellulitis again by:
- keeping skin clean and well moisturised
- cleaning any cuts or wounds, or using antiseptic cream
- preventing cuts and scrapes by wearing appropriate clothing and footwear
- wearing gloves if working outside
Cellulitis complications
If not treated quickly, the infection can spread to other parts of the body, such as the blood, muscles and bones.
Emergency action required: Call 999 or 112 or go to your emergency department (ED) if:
you have cellulitis with:
- a very high temperature or you feel hot and shivery
- a fast heartbeat or fast breathing
- purple patches on the skin
- feeling dizzy or faint
- confusion or disorientation
- cold, clammy, pale skin
- unresponsiveness or loss of consciousness
These are symptoms of sepsis. This can be very serious and life-threatening.
Content supplied by the NHS and adapted for Ireland by the HSE
