Athlete's foot is a common fungal infection that affects your feet. You can usually treat it with creams, sprays or powders from a pharmacy.
Athlete's foot can come back after treatment. But there are things you can do to reduce the risk of the infection coming back.
Symptoms of athlete's foot
A common symptom of athlete's foot is itchy white patches between your toes. But athlete's foot may not look the same on everyone.
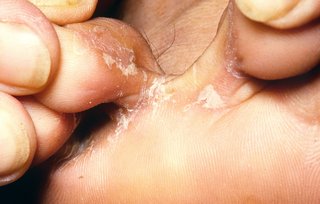
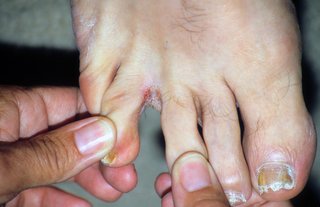
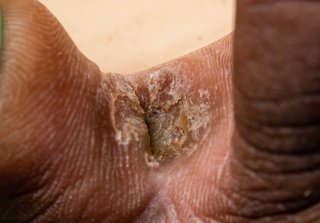
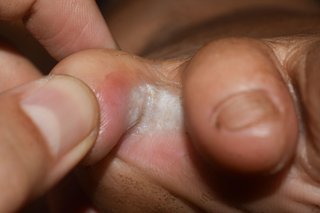
![A red crack in the skin at the base of a toe. The skin on the edge of the crack is wet and white. The skin around the crack has yellow flakes.]](https://assets.hse.ie/media/images/condition_athletes_foot_YByxn1H.width-320.jpg)
Other symptoms
You can get athlete's foot on the soles or sides of your feet. You can also get fluid-filled blisters.
If athlete's foot is not treated, it can spread to your toenails and cause a fungal nail infection.
Causes of athlete's foot
You can get athlete's foot if your skin comes into contact with the infection.
Contact with the infection can happen if you:
- walk barefoot in the same place as someone with athlete's foot, such as in a changing room or shower
- touch your foot against another person's infected skin
- share shoes or sock with someone who has athlete's foot
You are more likely to get an infection if the skin on your feet is wet, sweaty or broken.
Treatment for athlete's foot
Athlete's foot does not get better on its own. But you do not usually need to see a GP.
A pharmacist can recommend an antifungal medicine to treat or prevent athlete's foot.
The medicine usually takes a few weeks to work. Keep your feet clean and dry during and after treatment.
Antifungal medicines
Antifungal treatments for athlete's foot are available as:
- creams
- sprays
- powders
Always check the packaging or ask a pharmacist if a treatment is suitable for you. Some treatments are not suitable for children.
You might need to try a few treatments to find what works best for you.
Non-urgent advice: Contact a GP if:
- treatments from a pharmacy do not work
- your foot is red, hot and painful - this could be a more serious infection
- you have diabetes - foot problems can be more serious
- you have a weakened immune system - for example following an organ transplant
Further tests
Your GP may take a small sample of your affected skin cells. A laboratory can test the sample to find out what type of fungus causes your infection.
Your GP may
- prescribe a steroid cream and antifungal tablets
- refer you to a dermatologist (skin specialist) - if an infection is more serious
Things you can do yourself
There are things you can do to treat athlete's foot and stop it returning.
Do
-
dry your feet after washing them, particularly between your toes
-
pat your feet dry instead of rubbing them
-
use a separate towel for your feet and wash it regularly
-
take off your shoes when you're at home
-
wear clean socks every day - cotton socks are best
-
wear flip-flops or sliders in places such as changing rooms and showers
-
keep your shoes clean and dry
-
ask your pharmacist about antifungal powders for your shoes
Don't
-
do not scratch the affected area - this can spread the infection to other areas such as your groin or armpit
-
do not walk around barefoot
-
do not share your towels, socks or shoes
-
do not wear shoes that make your feet hot and sweaty
Content supplied by the NHS and adapted for Ireland by the HSE
