Week 28 until the birth of your baby is known as the third trimester. Your appointments with your GP, midwife or obstetrician will become more frequent in this trimester.
Your antenatal care
Tell your GP if you have not had a whooping cough vaccine during this pregnancy. It's best to have this vaccine within the first 36 weeks of your pregnancy. If you're more than 36 weeks pregnant there are still benefits but it might be less effective.
You'll also begin antenatal classes in preparation for birth and becoming a parent.
During the third trimester you'll decide on birth options and preferences. Your birth plans may have to change depending on how the pregnancy progresses.
Talk with your midwife or obstetrician before your due date to see what options are available to you.
Urgent advice: Talk to your midwife, obstetrician or maternity hospital immediately if:
- your baby's movements change, reduce or stop
It is not true that babies move less towards the end of pregnancy.
Braxton Hicks or uterine contractions
During late pregnancy your uterus (womb) may contract and relax. These are known as Braxton Hicks contractions.
Braxton Hicks contractions are different to labour contractions as they:
- do not happen as often
- are usually irregular
- do not last long - usually less than a minute
- do not increase in intensity
If you have Braxton Hicks contractions:
- walk around
- relax and take deep breaths
- call your GP, midwife, obstetrician or maternity unit if they do not stop or if they become more intense
Signs you're going into labour
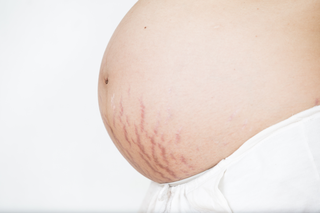
Stretch marks
You may notice pale pink or red narrow lines or streaks on your tummy, breasts and thighs. They may be itchy and feel tight. Almost 8 out 10 women get stretch marks during pregnancy.
There is no scientific evidence that creams or oils prevent stretch marks. If you are using them, make sure they are safe for pregnant women.
Keeping your skin well moisturised may reduce any itch or discomfort of the skin that some pregnant women experience.
Stretch marks will become white or silvery white over time. Most of the time they become hard to notice after your baby is born. Talk to a dermatologist if you feel self conscious about your stretch marks after the pregnancy. There are some treatments that might improve their appearance.
Heartburn and indigestion
Heartburn and indigestion can create a burning feeling in your chest and throat. It's caused by the pressure the growing baby is putting on your stomach, as well as hormonal changes.
Things you can do to avoid heartburn and indigestion:
- Eat smaller meals more often - larger meals may make the heartburn or indigestion worse.
- Try to eat healthier foods - fried foods may make your symptoms your symptoms worse.
- Avoid spicy or fried food.
- Avoid eating for 2 to 3 hours before you go to bed.
- Sleep propped up with lots of pillows.
- Talk to your pharmacist, GP, obstetrician or midwife about medicine.
Piles during pregnancy
Piles (haemorrhoids) can be painful and irritating when pregnant.
You may not have any symptoms from your piles.
If you do have symptoms, they may include the following:
- a lump, itching or pain around your bottom
- bleeding from your bottom - this is usually when you wipe your bottom after doing a poo
- pain when doing a poo
Things you can do to prevent piles:
- Eat foods high in fibre like oats, wholegrain bread and pasta, fruit and vegetables, potatoes with their skin on, peas, beans and legumes.
- Drink plenty of water.
- Avoid standing for long periods.
- Exercise.
Your pharmacist, GP or midwife can recommend a lotion for piles.
Healthy eating during pregnancy
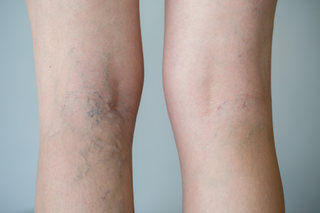
Varicose veins during pregnancy
Varicose veins are veins in the legs or vulva (the external part of your genitals) that have become swollen. They can be uncomfortable but they are not harmful and they usually disappear after birth.
Varicose veins can cause your legs to become:
- heavy or tired
- itchy
- swollen
- painful - you may get cramp or burning sensations
To reduce the swelling of your veins you can:
- try not to sit with legs crossed
- avoid standing or sitting for long periods
- sit with your feet up
- sleep with your legs higher than your body
- try compression tights - they can ease the symptoms of varicose veins, especially if you have to stand a lot at work
You can also reduce symptoms if you:
- eat a healthy diet and avoid gaining too much weight if possible
- take regular exercise - things like walking and swimming may help your circulation and improve or prevent varicose veins
Mental and emotional changes
It's normal to feel anxious about giving birth and becoming a parent.
As your baby grows you may be feeling uncomfortable. This can mean you feel more tired or irritable than usual. As your due date approaches it's normal to feel more anxious about the birth.
To reduce anxiety, remember to:
- trust your body - the processes in your body are doing exactly what they need to do
- talk to your partner, friends, family, and healthcare team
- tell your healthcare team if your anxiety is severe or prolonged
- keep your mind occupied by preparing for the birth, for example packing your hospital bag
You might find that you tidy and clean your home more than normal. This is common and is known as 'nesting'. When you prepare your baby's clothes and sleep arrangements you're likely to start feeling excited.