Piles are lumps inside and around your bottom (anus). They usually get better on their own after a few days.
There are things you can do to treat and prevent piles.
Non-urgent advice: Contact your GP
- if piles are causing you bleeding or pain
Piles are more common in pregnancy.
Symptoms of piles
Symptoms of piles include:
- bright red blood after you poo
- an itchy anus
- a feeling like you still need to poo straight after you’ve been
- slimy mucus in your underwear or on toilet paper after wiping your bottom
- lumps around your anus
- pain around your anus
See what piles look like
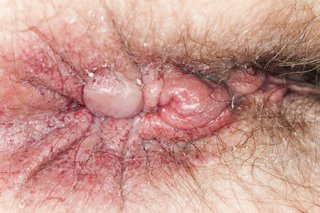
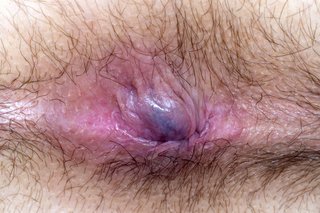
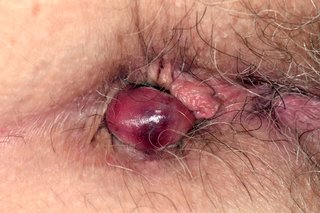
Treating and preventing piles
There are things you should do to treat and prevent piles.
Do
-
drink lots of fluid and eat plenty of fibre to keep your poo soft and easy to pass
-
wipe your bottom with damp toilet paper
-
take paracetamol if your piles hurt
-
have a warm bath to ease itching and pain
-
use an ice pack wrapped in a towel to ease discomfort
-
gently push a pile back inside
-
keep your bottom clean and dry
-
get regular physical activity and cut down on alcohol and caffeine to prevent constipation
Don't
-
do not wipe your bottom too hard after you poo
-
do not ignore the urge to poo
-
do not push too hard when pooing
-
do not take painkillers that contain codeine, as they cause constipation
-
do not take ibuprofen if your piles are bleeding
-
do not spend more time than you need to on the toilet
Ask a pharmacist about treatment for piles
Talk to a pharmacist to get advice on:
- creams to ease the pain, itching and swelling
- treatment to help constipation and soften poo
- cold packs to ease discomfort
You can ask the pharmacist to talk to you in a private area if you do not want to be overheard.
It can feel embarrassing to talk to your pharmacist or GP about piles. But piles are very common. Your GP is used to diagnosing and treating piles.
GP treatment for piles
Non-urgent advice: Contact your GP if:
- you have any bleeding from your bottom
- there's no improvement after 7 days of treatment at home
- you keep getting piles
Your GP may prescribe stronger medicines for piles or constipation. They can also check for more serious conditions.
Urgent advice: Ask for an urgent GP appointment if you have:
- piles and your temperature is very high or you feel hot and shivery and generally unwell
- pus leaking from your piles
Hospital treatment for piles
You might need hospital treatment if your piles do not improve after home treatments. If so, talk to your GP about the best treatment for you.
Treatment does not always prevent piles from coming back.
Treatment without surgery
Common hospital treatments for piles include:
- rubber band ligation - a band is placed around the piles to make them drop off
- sclerotherapy - a liquid is injected into the piles to make them shrink
- electrotherapy - a gentle electric current is applied to make the piles shrink
- infrared coagulation - infrared light is used to cut the blood supply to the piles and make them shrink
You'll be awake for this type of treatment, but the area around the piles will be numbed. You can usually go home on the same day.
You may need surgery to remove your piles if these treatments do not work.
Surgery for piles
Surgical treatments include:
- haemorrhoidectomy - the piles are cut out
- stapled haemorrhoidopexy - the piles are stapled back inside your anus
- haemorrhoidal artery ligation - the piles are stitched, which cuts off the blood supply to the piles and makes them shrink
You'll usually be asleep for the surgery. You may need to stay in hospital for more than a day.
Emergency action required: Phone 112 or 999 or go to your nearest emergency department (ED) if you have piles and you’re:
- bleeding non-stop
- bleeding heavily - for example, the toilet water turns red or you see large blood clots
- in severe pain
What we mean by severe pain
Severe pain:
- always there and so bad it's hard to think or talk
- you cannot sleep
- it's very hard to move, get out of bed, go to the bathroom, wash or dress
- you cannot work due to the pain
Moderate pain:
- always there
- makes it hard to concentrate or sleep
- you can manage to get up, wash or dress
Mild pain:
- comes and goes
- is annoying but does not stop you from doing things like going to work
Causes of piles
Piles are swollen blood vessels. It's not clear what causes them.
You’re more likely to get piles if you:
- are constipated
- push too hard when pooing
- are pregnant
- lift heavy objects
Piles during pregnancy
Piles are more common during pregnancy. You're more likely to get piles if you’re constipated (having trouble pooing).
Ask your GP or obstetrician for a stool softener (medicine to soften your poo) if you are constipated during your pregnancy.
Preventing constipation
To avoid becoming constipated:
- drink lots of fluids - you need 2 extra glasses of water a day if you're pregnant
- include plenty of fibre in your diet, such as fruit, vegetables and wholegrains
Content supplied by the NHS and adapted for Ireland by the HSE
