Measles is a viral infection that spreads very easily.
Get the measles, mumps and rubella (MMR) vaccine to avoid getting measles. Do not get the vaccine if you are pregnant.
Check if you or your child has measles
Measles starts with cold-like symptoms around 10 days after you get infected.
The first symptoms of measles are:
- cold-like symptoms such as aches and pains, a runny nose, sneezing and a cough
- sore, red eyes that may be sensitive to light
- a temperature of 38 degrees Celsius or above (fever)
- small grey-white spots in your mouth
- loss of appetite
- tiredness, irritability and a general lack of energy
You get a measles rash a few days later.
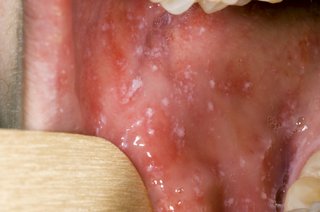
Small grey-white spots in your mouth
Not everyone with measles has these spots. The spots usually appear before the measles rash. If you have these spots and other symptoms or a rash, it's very likely you have measles.
The spots usually last for a few days.
The measles rash
The rash appears around 2 to 4 days after your first symptoms. It fades after around a week.
It usually starts on your head or neck and then spreads outwards to the rest of your body.
The rash can be flat or slightly raised and join together into large blotchy patches. It looks brown or red on white skin. It may be harder to see on brown and black skin.
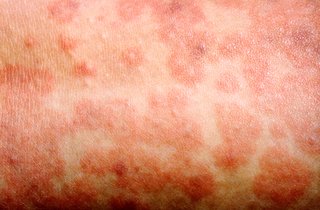
The rash is slightly itchy for some people. You will feel most ill on the first or second day after you get the rash.
Urgent advice: Contact your GP or maternity hospital urgently if you:
- are pregnant and you think you might have measles
- think you or your child has measles
- were in close contact with someone who has measles and you are pregnant
- were in close contact with someone who has measles and you did not have measles in the past or 2 doses of the MMR vaccine
Call before you go to your GP or hospital. They may need to make arrangements to reduce the risk of spreading the infection.
If you're not sure it's measles
You're unlikely to have measles if you had:
- 2 doses of the MMR vaccine
- measles in the past
The measles rash may look like other childhood conditions, such as roseola, rubella or slapped cheek syndrome.
How to treat measles
Measles usually lasts 7 to 10 days.
To ease your symptoms:
- take paracetamol or ibuprofen for the fever, aches and pains - do not give aspirin to children under 16 years old
- drink plenty of fluids to avoid dehydration
- close the curtains to lower your sensitivity to light
- use damp cotton wool to clean under you or your child's eyes
In severe cases, you or your child may need to go to hospital for treatment.
Emergency action required: Call 112 or 999 or go to your nearest emergency department (ED) if
you or your child has measles and:
- shortness of breath
- a sharp chest pain that feels worse with breathing
- cough up blood
- are drowsy
- confusion
- fits (convulsions)
These symptoms may be a sign of a serious bacterial infection.
Tell the operator that you have measles or call before you go to an ED. The hospital may need to make arrangements to reduce the risk of spreading the infection.
How to avoid spreading measles
Measles spreads when an infected person coughs or sneezes. There are things you can do to reduce the risk of spreading it.
Tell your child's school or childcare if your child has measles. Children in your child's group or class may need to get the MMR vaccine.
Do not go to work, school or childcare until at least 4 days after you first got the measles rash.
Avoid contact with young children, pregnant women and people who have a weak immune system.
How to avoid getting measles
When you get measles, your body builds up immunity to the virus. It's very unlikely you'll get measles again.
Measles vaccine (MMR)
You or your child can avoid getting measles by having the MMR vaccine. The MMR vaccine is offered to all children in Ireland. You get 2 doses.
If you were in close contact with someone who has measles
If you were in close contact with someone who has measles, call your GP for advice.
They can tell you about treatment to reduce your risk of developing measles. This can include an MMR vaccine or human normal immunoglobulin (HNIG).
Most people do not need HNIG. Your doctor can tell you if this treatment is recommended for you.
It may be recommended for:
- babies under age 6 months
- pregnant women who did not have 2 doses of the MMR vaccine or measles in the past
- people with weak immune systems - for example people living with HIV or having treatment with chemotherapy or radiotherapy
HNIG should be given within 6 days of exposure.
Complications of measles
Measles usually passes without causing any serious problems.
Common problems that can be caused by measles include:
- diarrhoea and vomiting
- a middle ear infection
- conjunctivitis
- inflammation of your voice box (laryngitis)
- infections of your airways and lungs, such as pneumonia
- fits caused by a fever (febrile seizures)
Measles can lead to serious problems if it spreads to other parts of the body, such as the lungs or brain.
Rare problems that can be caused by measles include:
- inflammation of your liver (hepatitis)
- eye disorders and vision loss
- meningitis
- a brain infection
- heart and nervous system problems
Some people are more at risk of having problems because of measles.
These include:
- babies under 1 year
- children with a poor diet
- people with a weak immune system, such as those with leukaemia
- teenagers and adults
Children who are older than 1 year have the lowest risk of having problems because of measles.
Measles in pregnancy
If you get measles when you're pregnant and you're not immune to it, it could harm your baby.
It can cause:
- miscarriage or stillbirth
- premature birth
- low birth weight
Urgent advice: Call your GP or maternity hospital urgently if
you are pregnant and you:
- think you were in contact with someone who has measles
They can tell you about treatment to reduce your risk of developing measles.
Call before you go to your GP or hospital. They may need to make arrangements to reduce the risk of spreading the infection.
Content supplied by the NHS and adapted for Ireland by the HSE
