Colposcopy takes about 15 to 20 minutes and you can go home the same day. It is ok to drive afterwards.
The examination is done in the same way as a cervical screening test. You will not have an anaesthetic.
Colposcopy should not be painful, but it can sometimes feel uncomfortable. A nurse will be there to provide support. They'll answer any questions you may have.
Preparing for colposcopy
Dos
-
Try to eat something before your appointment - you can eat and drink as normal.
-
Bring a panty liner with you - you may have some light bleeding or discharge afterwards.
-
Bring a friend or relative with you to the hospital if you think it will help.
-
Talk to your GP when you get your appointment if you have vaginal dryness or vaginal atrophy. They will tell you what steps you can take before you have the test done to make it more comfortable, such as using oestrogen gels and creams.
At least 24 hours before your appointment:
Don'ts
-
do not use vaginal medications, lubricants, creams or pessaries
-
do not have sex
-
do not use tampons or menstrual cups
-
do not wash inside your vagina (douching)
Contact the colposcopy clinic before your appointment if you:
- have your period - you may need to reschedule your appointment
- are pregnant - a colposcopy is safe but you may have to delay treatment
- want the examination done by a female doctor or nurse
It is safe to attend with your coil in. But there is a small risk the strings may be cut. The colposcopist will discuss this with you.
The colposcopy examination
Colposcopy is done by a specialist called a colposcopist. This may be a doctor or a nurse.
Before the colposcopy examination, they will:
- ask you about your medical history
- explain what a colposcopy is
- explain treatments for abnormal cell changes
- explain any risks linked to the treatment
- ask for your consent
During the examination:
- You undress from the waist down - you may not need to remove a loose skirt. But you will need to remove your underwear.
- You lie down on an examination bed.
- A device called a speculum is gently put into your vagina - this is like having a cervical screening test.
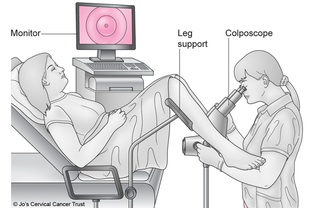
- A microscope with a light (a colposcope) is used to look at your cervix. This stays outside your vagina. It allows the colposcopist to see the cells on your cervix.
- The doctor will use a special dye on your cervix to highlight any abnormal areas.
- They might take a small sample of tissue (a biopsy) for closer examination in a lab. This should not be painful, but you may feel a slight pinch or stinging sensation.
You can ask for the exam to be stopped at any time.
After colposcopy
After having a colposcopy examination you:
- will be able to go home as soon as you feel ready, usually straight afterwards
- can return to your normal activities immediately, including work and driving
- may have a brownish vaginal discharge, or light bleeding if you had a biopsy - this is normal and should stop after 3 to 5 days
- should wait until any bleeding stops before having sex or using tampons, menstrual cups, vaginal medications, lubricants or creams
You may need to return for follow-up visits. If you do, your doctor or nurse will let you know.
How to reduce the risk of infection after a biopsy or treatment
Treatment on the same day
If abnormal cells are clearly found, you may be offered treatment to remove the cells immediately. In some cases, you'll need to wait until you get your biopsy results.
If you have treatment on the same day as your examination, you will need to take things easy for the rest of the day.
Your doctor or nurse will tell you what you need to do after treatment.
Treatment and post-treatment care
Risks and side effects
Colposcopy is very safe. It should not cause any serious problems.
But you may have:
- discomfort or pain - tell the colposcopist if the examination is painful, they will try to make you more comfortable
- brown or black vaginal discharge - this can be caused by the dye or paste that may be used after a biopsy and should pass quickly
- light bleeding - this can happen if you have a biopsy and should pass within 3 to 5 days
Urgent advice: Contact the colposcopy clinic or your GP if you have:
- heavy bleeding or bleeding that does not go away
- smelly vaginal discharge
- a fever
- constant tummy pain
Content supplied by the NHS and adapted for Ireland by the HSE
