Hand, foot and mouth disease is a common childhood illness that can also affect adults. Most adults are immune. It is highly contagious. It usually clears up by itself in 7 to 10 days.
Hand, foot and mouth disease is not the same as foot and mouth disease. Foot and mouth disease affects farm animals such as cattle, sheep and pigs.
You cannot catch hand, foot and mouth disease from animals.
Check if it’s hand, foot and mouth disease
It can take 3 to 5 days for symptoms to develop after your child becomes infected.
Most of the time you can treat your child at home.
The first symptoms are:
- a sore throat
- a high temperature, above 38 degrees Celsius
- not wanting to take milk feeds or eat
After a few days, mouth ulcers and a rash will appear.
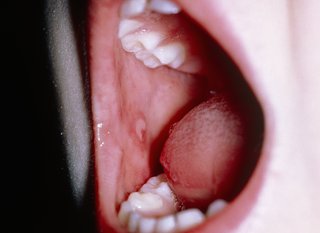
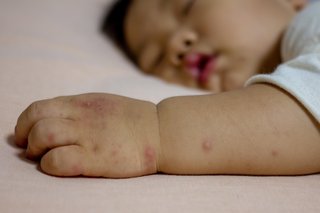
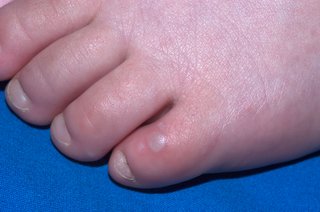
Symptoms can be the same in adults and children. They're usually worse in babies and children under 5 years.
You can get hand, foot and mouth disease more than once. But it's normally not as severe the next time.
Sometimes a rash combined with a high temperature can be a symptom of another serious infection such as meningitis. You can do a glass test to make sure it isn't.
How to treat hand, foot and mouth disease in children
To help with the symptoms:
- drink fluids often to prevent dehydration – avoid acidic drinks such as fruit juice
- eat soft foods like soup, mashed potatoes and vegetables, smoothies and ice cream
- avoid hot or spicy foods
- avoid acidic fruits like tomatoes and citrus fruits
- rinse your mouth with warm, salty water and spit it out. Only give this to your child if they are old enough to spit it out
If your child is unwell or uncomfortable with a fever, giving them paracetamol or ibuprofen can help. Only give your child ibuprofen if they are older than 3 months. Adults who are unwell can also take paracetamol or ibuprofen.
You cannot take antibiotics or medicines to cure hand, foot and mouth disease.
Talk to a pharmacist
Speak to a pharmacist for advice about treatments. Mouth ulcer gels, sprays and mouthwashes can help relieve pain.
They can tell you which ones are suitable for children.
Important
Aspirin should not be given to children under 16 years.
Ask a pharmacist about suitable medications for you or your child.
When to see your GP
You will probably know if you or your child has hand, foot and mouth disease without needing to go to a GP.
If there's an outbreak of the virus at your child's school or crèche, it's likely they've caught the virus.
Non-urgent advice: Phone your GP if:
- your child’s symptoms don't improve after 7 to 10 days
- your child has a very high temperature (above 38 degrees Celsius), or feels hot and shivery
- you're worried about your child's symptoms
- your child gets dehydrated – they're not peeing as often as usual
- you're pregnant and get hand, foot and mouth disease
Hand, foot and mouth disease is contagious. Check with your GP's surgery before going in-person.
They may suggest a phone consultation. This is to prevent the infection from spreading to other patients.
Test for hand, foot and mouth disease
Your GP or paediatrician may need to do other tests if they are not sure your child has hand, foot and mouth disease.
These could include:
- a swab - where they rub the back of your child's throat with a swab (this looks like a long cotton bud)
- a poo sample
These samples will be sent to the lab for testing.
Hand, foot and mouth disease in pregnancy
There's normally no risk to the pregnancy or baby. But, it's best to avoid close contact with anyone who has hand, foot and mouth disease.
This is because:
- having a high temperature during the first 3 months of pregnancy can lead to miscarriage, but this is rare
- getting hand, foot and mouth disease shortly before birth can mean the baby is born with a mild version of it
Speak to your GP or midwife if you have been in contact with someone with hand, foot and mouth disease.
Try not to worry. Adults are less likely to become infected than children.
Complications from hand, foot and mouth disease
Mouth ulcers caused by hand foot and mouth disease can make it hard to eat and drink.
Dehydration
A sore mouth or throat can make it difficult to drink and swallow. Drink plenty of fluids. Children can become dehydrated if they do not drink enough.
If their mouth is sore, your child may not want to drink. Giving them paracetamol or ibuprofen regularly can help with this. It might help to give them sips of fluid, using a straw.
If your child is breastfeeding, offer them regular breastfeeds. This will help them stay hydrated. It will also comfort them too.
If you or your child become severely dehydrated, you may have to be treated in hospital and be given fluids through a drip. A drip is a small tube placed into a vein in your child's hand or arm.
Infection
Talk to your GP if any of your child’s blisters start oozing pus or the skin around them becomes very red.
Serious complications from hand, foot and mouth disease
Serious complications due to hand, foot and mouth disease are rare.
In rare cases, the virus can cause inflammation of the heart, the brain or the lung. In very rare cases these complications can cause death.
Take your child to your nearest hospital emergency department (ED) that treats children if they have hand, foot and mouth disease and any of the following symptoms:
- dislike of bright lights
- headache
- stiffness in their neck
- drowsy (you find it hard to wake them)
- confusion
- seizures
- difficulty breathing
- vomiting
Causes of hand, foot and mouth disease
Hand, foot and mouth disease is caused by coxsackievirus.
It's easily passed on to other people. It's spread in coughs, sneezes and poo.
You can become infected if you touch the blisters, poo or saliva of someone with hand, foot and mouth.
How to stop hand, foot and mouth disease spreading
You're most likely to give hand, foot and mouth disease to others in the first 5 days after symptoms start.
To reduce the risk of spreading hand, foot and mouth disease:
- wash your hands often with warm soapy water, and teach children to do so
- use tissues to trap germs when you cough or sneeze
- bin used tissues as quickly as possible
- don't share towels or household items, like cups or cutlery
- wash soiled bedding and clothing on a hot wash
- wash your hands before preparing food
- do not put your child's soother in your mouth - for example, if it falls to the ground
Staying off school, pre-school or childcare
Keep your child off school, pre-school or childcare while they are feeling unwell.
As soon as they're feeling better, they can go back. There's no need to wait until all the blisters have healed.
Keeping your child home for longer is unlikely to stop the illness from spreading. Your child was probably contagious even before they had symptoms.
