Eczema is a condition that causes dry, red, itchy skin, Babies (including newborns) and children can get it.
Symptoms
The main symptom of eczema is itching. At night this can lead to disturbed sleep and irritability.
Your child's skin may look dry, cracked and sore. It may look like a rash.
If your child has white skin, eczema can make the skin red.
On black or brown skin, eczema can make the skin dark brown, purple or grey. It can be hard to see eczema on black or brown skin.
They may also have scratch marks and bleeding. Their skin may appear wet if it's inflamed or infected.
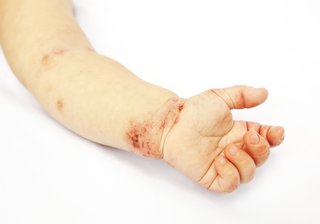
Eczema is usually found:
- on the face
- in the creases of necks, elbow joints and the backs of knees
- on hands
But any area of your child's skin can be affected.
Diagnosis
Non-urgent advice: Contact your GP if your child:
- has symptoms of eczema
Your GP can diagnose eczema by looking at the skin. Blood and skin tests are not usually needed.
Your GP may dab your child's skin with a swab (like a cotton bud) to see if the eczema is infected. This should not cause your child any pain.
Treatment
Your GP may prescribe:
- lotions, creams or ointments (emollients) to moisturise your child’s skin
- steroid creams - to help reduce itching and redness
- antihistamines - to reduce itchiness so that your child can sleep
- cotton bandages - to stop creams rubbing off and prevent your child from scratching
- antibiotics - if your child's eczema becomes infected
Moisturise your child's skin as often as possible, at least 3 or 4 times every day.
Non-urgent advice: Contact your GP if
your child has eczema and:
- is having a flare up that is not getting better after 2 to 3 days of regular treatment
- has oozing, crusted or broken areas of skin, or if the area around the eczema looks red or feels hot - their skin may be infected
- has symptoms that are worrying you
Using emollients
Lotions, creams or ointments used to moisturise your child’s skin are also known as emollients.
Emollients are very effective at treating dry skin conditions, such as eczema.
Warning
Keep away from fire, flames and cigarettes when you use any emollient.
How to help a child with eczema
There are things you can do to help ease your child's discomfort.
Do
-
keep their fingernails short to reduce the damage to their skin from scratching
-
wash them with a soap substitute, such as emulsifying ointment or Silcocks base
-
give them short, lukewarm baths - use a special bath moisturiser or whisk up some emulsifying ointment with water and add to the bath
-
pat them dry after a bath before smoothing on moisturiser to “lock in” moisture - be careful, as the bath may be slippy
-
use non-biological detergent and a double rinse cycle when washing their clothes or bedding
-
only use a cream recommended by your GP
-
shower them after swimming and pat skin dry with a towel in the direction of hair growth
-
dress them in cool, breathable fabrics, such as cotton
-
keep their room temperature at around 18 degrees Celsius
-
keep them away from anyone with a cold sore - the cold sore virus can cause eczema to become infected
-
use extra moisturiser on areas your child scratches a lot
Don't
-
do not use your fingers to take moisturiser out of tubs as you may introduce bacteria- use a clean spoon instead
-
do not rub your child with a towel as this may make eczema worse
Causes
Atopic eczema (atopic dermatitis) is the most common form of eczema.
It's not always known what causes atopic eczema.
Your baby or child is more likely to have atopic eczema if:
- 1 or both of their parents have it
- they or a close family member has asthma or hay fever
Eczema triggers
Some things can cause your baby or child's eczema to get worse, or 'flare up'.
These include:
- heat or changes in temperature
- coming into contact with an allergen or irritant such as soap, washing detergent, pets, some fabrics, pollen, house-dust mites or certain foods
- skin infections, such as a staph infection
- teething
- some viruses
- stress
Food allergies do not usually cause eczema. But skin that is already inflamed from eczema may be irritated by certain foods. Ask your GP to refer your child to an allergy specialist if you think they have a food allergy.
Keep a food diary to check if there's an obvious link between specific foods and eczema getting worse.
Do not cut food groups from your child's diet unless you’ve been advised to by a doctor or specialist nurse. This could affect your baby’s growth and development.
Allergies and weaning
